“Wev’e been here five and half hours. And we are still waiting for Dr. Meyers to come back to the room again”. This complaint was being lodged with the receptionist at the Vincera Institute. I smiled inwardly. I remembered that first appointment. Indeed, between the two MRIs performed and the three doctors I met with it was a 5 hour visit. . . and you know what? I left with answers from a caring team of medical professionals. I guess patients have gotten used to the quick usual answer of “rest and take this medication and all will be well”.
But that isn’t what brings one to visit Vincera Institute. It is certainly not what brought me here. What brought me was a lot of unanswered question after countless X-Rays, an MRI, and an ultrasound along with several different doctors. I thought about this as I contemplated my choices while I waited in the lobby to see Dr. Meyers and his esteemed colleague Dr. Coleman.
After all the testing and my prior visit with Vincera, I knew what the issues were and why I had constant, pulling discomfort in the groin and hip area. Contrary to the first MRI where it did seem as though I was going to give birth to
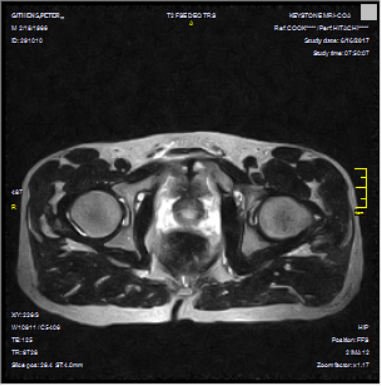
ET, the staff at Vincera had discovered a Core Muscle Injury (formerly known by me as athletic pubalgia, formerly known by all as the dreaded but poorly-named sports hernia.) Additionally, and perhaps causally, they found a fairly significant hip labrum tear in my left hip. Problem identified. Let’s fix it. I won’t re-bore you with the tale of insurance woes. Basically, I’m paying out of pocket to fix this.
So . . That brings me to Monday, October 16th and an afternoon pre-op appointment with both Dr. Meyers and Dr. Coleman. I’d been waffling constantly about whether to do both the hip and the pelvic floor repair (the repair of the core muscle injury). It really came down to money. If it were unlimited I’d have already had both repairs done. But I hadn’t actually met with Dr. Coleman yet and figured I was far enough in I may as well talk to him and get his opinion.
The office was running a bit behind. This was apparent by the complaint of the gentleman when I first arrived. Honestly, I was okay with this. I know why they are behind. Dr. Meyers and his staff take the time for thorough examinations, thorough interviews, and they take their time examining MRI and other test results. They want you to have an answer and your set of choices when you leave the office.
Today was no different but eventually we were taken back to an exam room where I would first meet with Dr. Coleman. Dr. Struan Coleman is my age almost to the month. His birthday is one month before mine. It’s as though we are brothers, except he is a rich, good looking doctor and I am . . Well I’m not.
After an examination, Dr. Coleman produced a little 3D model of the hip. It turns out I was predisposed from adolescence to some form of hip/groin injury. My hip ball was a bit misshapen causing a hitch which stresses the labrum. This hitch puts undue strain on the adductor which begin to pull off the pubic bone at their attachment point. I believe the only time I was ever aware of any sort of hitch in my hip was at the 2016 Boston marathon when my left hip began locking up inexplicably. Dr. Coleman believed that the hip caused the CMI and worried if we didn’t do both that I would continue to struggle. I could also have other problems related to the hip as I grow older including more severe arthritis, and early need for hip replacement. He wasn’t trying to scare me or force a choice and suggested I could try the CMI first and see if that was good enough, but a second surgery would ultimately mean another round of anesthesia which is always the biggest risk in surgery. Dr. Coleman left the room having provided all the information he could for me to make an educated decision.
It turns out I was predisposed from adolescence to some form of hip/groin injury. My hip ball was a bit misshapen causing a hitch which stresses the labrum. This hitch puts undue strain on the adductor which begin to pull off the pubic bone at their attachment point. I believe the only time I was ever aware of any sort of hitch in my hip was at the 2016 Boston marathon when my left hip began locking up inexplicably. Dr. Coleman believed that the hip caused the CMI and worried if we didn’t do both that I would continue to struggle. I could also have other problems related to the hip as I grow older including more severe arthritis, and early need for hip replacement. He wasn’t trying to scare me or force a choice and suggested I could try the CMI first and see if that was good enough, but a second surgery would ultimately mean another round of anesthesia which is always the biggest risk in surgery. Dr. Coleman left the room having provided all the information he could for me to make an educated decision.
Dr. Meyers came in next. It had been more than two months since he saw me and I didn’t expect him to remember me. He sees a lot of patients. But he did remember. I’m sure he reviewed my chart but he remembered details that wouldn’t be in my chart. This was also the first he had met Janice and he took the time to introduce himself to her and explain his background.

We then got on with examination similar to that done last time including observing me while I removed my jeans. To be able to do this I had to lean against something when I lift my left leg as trying to balance hurt and was impossible. Janice knew he was observing what I had to do to get undressed.
After the examination, and a consultation with Dr. Coleman, and reviewing my MRIs, Dr. Meyers pointed out the decisions for what to do were all mine. “There isn’t any pressure here but I’m worried if we don’t fix both problems that the solution won’t work for you. However, I’ll do whatever you decide. And it could work out just fine”.
I had already decided I was doing the pelvic floor repair but I was back on the fence about the hip. I thought fixing both was the appropriate thing to do, Janice thought so, and so did Dr. Meyers and Dr. Coleman. I went to see Marcia to finish up some pre-op paperwork including paying for Dr. Meyers. (Ouch.) She then referred me to Alberto who was Dr. Coleman’s assistant to learn about Dr. Coleman’s fee. (Double ouch . . So far this was pretty painful surgery and a knife hadn’t touch my skin yet).
We were working under the assumption until I said otherwise that we would do both fixes in surgery the next morning. I went upstairs to get fitted for crutches, and a hip brace “just in case I’m doing the hip”. I also met Sarah, a physical therapist, who did some preoperative training. She showed me how to get on and off the table or bed, and how to walk on crutches. Again, these would all become necessary if I got both the hip and pelvic floor repairs.
After seeing Sarah, I tracked down Dr. Meyers and asked him one more time. “If I want to get back where I was prior to this injury, able to run fast and far, drive and sit without discomfort, operate in everyday life without discomfort you think my best chance for success is to do both repairs. Correct?” Dr. Meyers without hesitation said “YES”. Okay . . It’s only money. Let’s do it. It seemed silly to do anything less.
I let Marcia know my final decision and wrote Alberto a check to cover Dr. Coleman’s portion of the surgery, then took my fancy new hip brace and Janice and I left for Rite Aid. I had been given a prescription for Percocet that they recommended filling beforehand. That was an interesting prescription fill. There is much more information required for an opiate-based pain killer these days than a few years ago. My hope was not to have to use too much of them. On a funny side note, the prescription was for 50 pills. My cracker jack insurance would only pay for 48. Go figure.
Once we had the script, we returned to the grounds of the old Philadelphia Navy Yard where Vincera is located, and checked in to the Marriott which is just a couple blocks away. We kept things simple and had dinner in the hotel and turned in. I was to arrive at the surgery center at 5:30.

I must say that everything about Vincera Institute is clean, and state-of-the-art. The staff are super friendly and patient. The surgery center experience was no different. After I was checked in, I was taken to the prep area by a nurse named Alex who got all my vitals, put in the IV and made sure I was warm before retrieving Janice to sit with me until surgery started. During this time, Drs. Meyers and Coleman came in and took sharpie to my body to mark the appropriate places to cut or not cut. I also met Matt the anesthetist, and the nurse anesthetist Kristin.
Eventually I was wheeled into the OR. The last time I was in an OR was some 40 years ago.  The new ones look a lot nicer. That last time I was having some sinus surgery done since nobody could figure out why I was always having respiratory issues and my sinuses had developed some scar tissue. All these years later, I learned I’m very allergic to cat dander. Since I nearly always had a cat that may have explained those childhood issues. Wait . . Where’d the story go? Oh, right. Operating Room. First, one more tale from that early operation. I remember them sticking the pads to my chest and turning the machine on and it flat-lined. The last thing I saw before going under was someone whack the machine with their hand and it started reading properly. I remembered hoping that if it flat-lined again someone would remember to give it another whack.
The new ones look a lot nicer. That last time I was having some sinus surgery done since nobody could figure out why I was always having respiratory issues and my sinuses had developed some scar tissue. All these years later, I learned I’m very allergic to cat dander. Since I nearly always had a cat that may have explained those childhood issues. Wait . . Where’d the story go? Oh, right. Operating Room. First, one more tale from that early operation. I remember them sticking the pads to my chest and turning the machine on and it flat-lined. The last thing I saw before going under was someone whack the machine with their hand and it started reading properly. I remembered hoping that if it flat-lined again someone would remember to give it another whack.

But back to present day. The new OR looked like a room on the International Space Station. There were people buzzing about. An oxygen mask was placed over my face. Matt or Kristin were there and said something about medicine.
“Hi there. It’s all over.” Said a very caring voice as my eyes opened. My throat was a little dry and my lower abdomen hurt more and more as I came to. Tanisha, my recovery nurse, acted quickly administering a shot of Fentanyl. I see why it is a popular street drug. Almost instantly the pain was gone. Tanisha assured me it doesn’t last long and I should eat something so she could give me Percocet. She brought some apple juice and some chocolate chip cookies. My mouth was so dry I had to take little bits of cookie and moisten my mouth with apple juice to swallow. But I did get down 3 cookies, enough to have a dose of Percocet as the Fentanyl wore off.
Tanisha went and retrieved Janice. Dr. Meyers had completed his part of the surgery first and had called on her phone to provide an update. His portion had gone well and he explained that I had a major tear on the left side. This isn’t a surprise to me. I’ll confirm with the doctor later but I don’t believe there is any therapy or alternative treatment that could be used to solve this aside from the surgery. Shame on you American healthcare system. Shame on you indeed.
Once I was awake and had a snack and the Percocet I was ready to get dressed and head upstairs to see Sarah. Getting dressed didn’t sound like much fun. But Tanisha and another recovery nurse dove in helping me get on compression shorts (recommended for swelling) warm-up pants, socks, shoes, and shirt. Then it was time to sit up and navigate into a wheel chair. This was not the most fun thing but we got it done. Then it was up the elevator and into rehab where Sarah applied a Game Ready device that massaged the affected areas with cold for twenty minutes.
It was sometime around 3:00 when the Vincera folks helped me into the car and Janice drove us off in search of something to eat. Fortunately, I had no nausea from the general anesthesia which I guess is fairly common. I didn’t know it yet but the only side effect I would really suffer from was an inability to urinate. Apparently, they may ask you to try to do this in recovery but I hadn’t had to because they had a catheter in for surgery so I was pretty empty. It would be hours before I’d feel the need to pee.
In the meantime, my appetite was good. We grabbed a couple sandwiches from a nearby South Philly steak shop and I found a Termini Brothers bakery location not far away where we grabbed a little treat. Then back to the hotel where I ate with a dry mouth. The sandwich was good but required a lot of water to be able to swallow it. I spent most of the rest of the afternoon in and out of naps. Between lingering anesthesia, and the Percocet, I was wiped out.
About 6:00pm I decided I had to pee. At risk of TMI . . Despite my best efforts not much happened. Uh oh. I tried again every so often with minimal effect. I texted Dr. Meyers (he gives you his cell number). We agreed that if things came to a complete stop I’d head to the ER. Fortunately, throughout the night I was able to go enough to not have a lot of pressure or discomfort. Just a little bit at a time. In between I’d fall into a Percocet induced sleep. Every 30 minutes or so I’d get up to go as best as I could and decided if things didn’t get better by morning I’d text Dr. Meyers again.
But they did! I’ve said it before. Never take the little things like peeing for granted. Now if only Sarah and I had reviewed how to be able to sit on a toilet. But that’s definitely TMI.
Today I go back to see Sarah for the initial PT visit which I’ll continue with my go-to PT, Vanessa Bowers starting next week. I’ll also have follow up with Dr. Meyers today and then we’ll head for home.
So the summary is, things seem to have gone well. I’m a bit sore but, oddly, even at it’s worst yesterday the pain was not as bad as what I had at the end of the Boston Marathon this year after running 26.2 miles with this injury. Now I have two and half months of rehab mostly for the hip. At the end of which I should be as good or better than before. I just hope I can hold on to my swim, bike, run mojo at that point. You can also bet there will be a lot more core work to keep things healthy and strong too.


I’m glad it all went well Pete! Injuries are no fun – just ask JJ Watt, he won’t lie to you. Do your PT, stay within their limits when you are not actually at PT, and in no time – like around May of next year….It will all be a distant memory. Yes, I know you said 2 and half months of rehab. It then takes another 4 and a half months to get back to where you can train/move/live like you used to. Muscle atrophy is a LOT faster than muscle building!! Ask any bodybuilder……They know. Hang in there, with any luck, it’ll all turn out how you hoped.
Actually the goal at Vincera is to have you back to where you were or better at the end of rehab. That is there measure of success.
Hi,I had a hernia problem and that ended with surgery. Quality repair is essence of good recovery and please educate yourself so you can prevent surgery or worsening of health ,this article is perfect example. Thanks for such detailed defined article and sharing these useful information’s
Thanks John!
Did Dr Coleman do a labral repair and fix the impingement or just fix the tear?
How is your exercise level now?
Hi Amy . . sorry I just saw this. Dr. Coleman fixed both the impingement and the labral tear. The labrum fix included anchoring the repaired labrum to the hip bone. At the end of the blog I mentioned 2.5 months of rehab. That was wrong. Recovery time from the combination surgery is 3-6 months depending on the person. I las saw Dr. Coleman in late December. He was pleased with my progress, said I’m ahead of schedule and gave me the greenlight to increase cycling time and effort, add in swimming, and to begin running 3 month after surgery. Tomorrow is the 3-month mark. The suggestion was to start out with a walk/run mixture on the treadmill and increase gradually. I put that off a week due to some soreness I’ve had for a couple days. It is minor and I think it is probably just some scar tissue. Overall, I’m very please with outcomes so far and am optimistic about getting back to much stronger, better running and other activities.
I hope you heal well! I’m glad you got quality care and did what you needed to. It’s a tough decision but I am sure you’ll be happy you did it!! 🙂
Thanks Jenna. Time will tell. So far rehab is going well. I have some occasional soreness but less and less. I’m still working with my therapist and hope to add running back in to the mix very soon. I won’t know for sure that everything was a success for a few weeks or maybe months yet.
This may be insanely crass but can you divulge to cost of all of this? I have talked to the office and understand it is out of pocket, in full (no financing) and then one can work on reimbursement from insurance company. But I cannot seem to get answer of what is guesstimate of total cost…initial appointments, MRIs, cost of surgery, anesthesiologist , meds PT.
Hi Erin. Shoot me an email. I’ll be happy to share with you what I had to pay. Pgithens@ptd.net
Thanks. Sent you an email.
Thank you for posting this information Pete. It’s priceless for knowing what to expect. Very interested to hear about your recovery and challenges! Important thing to remember is as we get older we do not heal as fast, or as well as a teenager, or an all star major league baseball pitcher. So hearing about your recovery progress is great information. Wishing you all the best!
Thanks Phil. I did have a bit of mis-information in that entry I should fix. Recovery including the hip is 3-6 months. It has gone extremely well and I’m just about at the 6 month juncture now and very much returning to normal. I’m still working on re-establishing my run base but doing so without pain or discomfort at this point.
Hi Pete,
Our daughter is 12 years old. Since 2017 we have been looking for why she was having so much abdominal pain. 7 months in 2017 she was out of school half of a year. Then this year she was put 3 1/2 months, admitted to the hospital twice , work ups from Gynocologist, Gastroenterologist, family doctor, physiatrist….. full work ups. Nothing came up. They were giving up and relating the pain to either stress or nerve issues. Trying to Medicate her. Nothing helped. We found Vincera not thinking she had any type of core injury. It NEVER CROSSED OUR MINDS. NEVER. We canceled our appointment at CHOP in Philly and decided to take this chance. She was In pain 24/7. It was just unbelievable.
Long story short, we went to get our MRI and Xrays and met with Dr. Meyers to discuss the results. Our daughter needed surgery the next day. She had tears that were healing/ scabbing along with adhesions. She had an umbilical hernia. She had new tears both sides, nerves were so compressed, under the muscle ,especially on the right where most of her pain was. Her pelvic muscle was also tearing away from the bone. We were in complete and utter shock. This was never even looked into for over 11 months of a child not even able to stand for two hours a day. Dr. Meyers did surgery and she woke up without the pain she had. It was amazing. Today is day 11 post op. She started going back to school half days. It was such a hard day and she feels terrible after. My question to you is …. how much is to much….? I feel we are Pushing her back way to soon. How long did it take you to go back to regular daily activities? She is in bed now and feels terrible. Pain. Swollen. Said she feels popping. Thank you so much for your guidance. I could really use another opinion from someone who has been through this.
Sincerely,
Jennifer Kandl
First of all I’m so sorry your daughter has had such a difficult time but glad Dr. Meyers was able to help. I may not be the best litmus test to gauge against since it sounds like her CMI and umbillical hernia were much worse than mine. I had pain all the time as well but not nearly as severe. Also, since I had the hip labrum repair as well that was really a limiting factor for me. The pain from that was worse but more it limited what I was able to do for much longer so delayed my return to activity. In fact, the problem with that is the CMI heals faster than the hip labrum and they start to worry about scar tissue.
That said, other than when I woke up from surgery, I don’t remember having a great deal of pain from the CMI repair. If you haven’t done so, I’d recommend calling Dr. Meyers and talking to him. Good luck and I hope your daughter is pain free very soon!
(sorry meant to reply to Pete) here are my questions:
are you able to start running? how is your hip surgery recovery going?
are you able to start running? how is your hip surgery recovery going?
Hi Allie
The surgery and recovery were the best things I could do. No more constant pain and I’m free to run again.